- Last edited on March 14, 2024
History of the DSM
Primer
The DSM (Diagnostic and Statistical Manual of Mental Disorders) has a long and storied role in the history of psychiatry. As the cornerstone of Western psychiatry and guide for millions of clinicians and healthcare providers, it has been the most significant advance in the diagnosis and treatment of mental disorders. However, in the midst of its success, important criticisms of its role have also arisen.
But the unifying and synthesizing whole of DSM-IV is still worth much more than would be the accumulated sum of its individual parts. However imperfect, the DSM's special value is as a common denominator that avoids a Babel and is good enough (if admittedly not best) at each of its jobs.”
– Allen Frances, MD, Chair of the DSM-IV Task Force

PsychDB is an Amazon Associate and earns from qualifying purchases. Thank you for supporting our site!
The Cycle of Classification: DSM I through DSM-5
Blashfield, R. K. et al. (2014). The cycle of classification: DSM-I through DSM-5. Annual review of clinical psychology, 10, 25-51.Pre-DSM Era
The origins of the DSM starts in the 1800s, when first official attempts were made to try to gather information about mental health in the United States. Government officials tried to record the frequency of “idiocy/insanity” in the 1840 census. By the late 1800s, mental health categories included mania, melancholia, monomania, paresis, dementia, dipsomania, and epilepsy.[1]
In 1921, the American Medico–Psychological Association became what is now known as the American Psychiatric Association (APA), and developed the American Medical Association’s Standard Classified Nomenclature of Disease. This early classification system was designed for diagnosing inpatients with severe psychiatric and neurological disorders.
DSM-I
The DSM-I owes it origins to post-war America. After World War II, the World Health Organization (WHO) published the 6th edition of International Classification of Diseases (ICD-6), which had a section on mental disorders for the first time. The ICD–6 was heavily based on the U.S. Veteran's Administration classification and included 10 categories for psychoses and psychoneuroses, and 7 categories for disorders of character, behaviour, and intelligence. Shortly after, the APA developed a variant of the ICD–6 that was published in 1952, the first edition of the DSM (DSM-I). The DSM-I became the first official manual and glossary of mental disorders with a focus on clinical use.
DSM-II
The DSM–II, published in 1968, was similar to DSM-I with its basis in psychoanalytic theory, but eliminated the term “reaction.” Even though the DSM II was published in more than half a century ago, the following excerpt is sage advice even (and especially) today.
A Tip From the DSM-II...
“The diagnostician, however, should not lose sight of the rule of parsimony and diagnose more conditions than are necessary to account for the clinical picture. The opportunity to make multiple diagnoses does not lessen the physician's responsibility to make a careful differential diagnosis.”DSM-III
The DSM–III, published in 1980, initiated the start of “modern psychiatric diagnosis.” Unlike the DSM-II, it took an agnostic approach to the etiology (causes) of mental disorders and instead focused on explicit diagnostic criteria. Attempts were made to construct and validate diagnostic criteria so that diagnoses could be reliably made between different clinicians. The DSM-III was heavily based on several influential papers, first by the Feighner Criteria, published in 1972 by Dr. John Feighner, which described diagnostic criteria for depression, schizophrenia, anxiety neurosis and antisocial personality disorder.[2] These criteria in turn greatly influenced the development of the Research Diagnostic Criteria (RDC), developed by psychiatrist Dr. Robert Spitzer.[3] Many of the diagnostic criteria familiar in the DSM-5 has its origins in these two influential papers.
The DSM-III can arguably be said to be the document responsible for ushering in the biological psychiatry era by standardizing diagnostic reliability. The ability to reliably diagnose the same disorders between clinicians made randomized control trials for medications and biological treatments much easier (for better or for worse).
DSM-IV
The DSM–IV, published in 1994, continued to build on the etiology-agnostic framework of the DSM-III. The APA working groups attempted to create a firm empirical basis for making modifications to existing criteria. At the same time, the authors of the DSM–IV also attempted to harmonize the diagnostic criteria with the 10th edition of the ICD (ICD-10).
DSM-5
Work on the DSM-5 began in 2000, with its publication finally occurring in 2013. One of the initial goals of the DSM-5 was to finally include biomarkers in its diagnostic criteria. However, this did not become a reality. The DSM-5 was in general criticized for expanding diagnostic criteria and labels.
Field Trials and Interrater Reliability
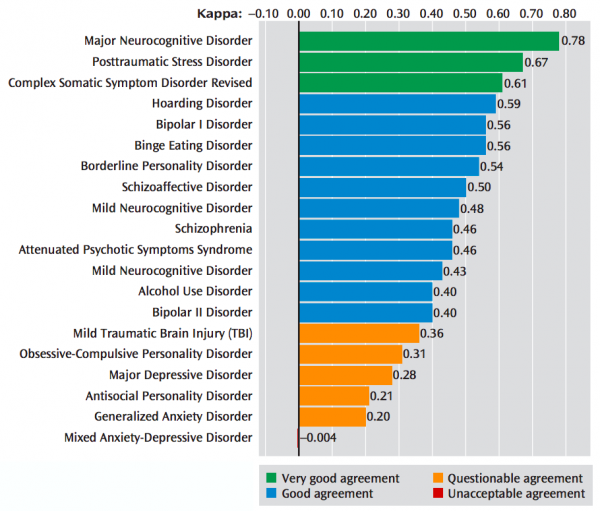
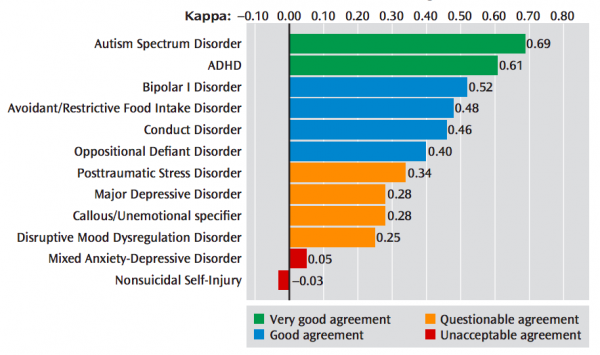
The DSM-5 field trials showed the inherent limitations of the DSM's etiologically agnostic approach to diagnosing mental disorders. Some disorders had good interrater reliability (e.g. - major neurocognitive disorder and posttraumatic stress disorder), while others were very poor. The most prominent example is for major depressive disorder, which has a very poor kappa = 0.28 (questionable agreement). One common reason is because the criteria covers a wide range of illness severity, and is a heterogenous condition.[4]
What is the Kappa Statistic?
Many medical diagnostics (e.g. - physical exams, imaging, and other diagnostic tests) often depend on some subjective interpretation by the observers. This is especially true in psychiatry where there are no objective diagnostics, and the clinician is the the diagnostic tool. Thus, the kappa statistic (or kappa coefficient) is the most commonly used statistic to measure the agreement between two or more observers. A kappa of 1 indicates perfect agreement between observers, whereas a kappa of 0 indicates agreement equivalent to chance. As an example, if an illness appears in 10% of a clinic's patients and two clinicians agree on its diagnosis 85% of the time, the kappa statistic is 0.46 (this is similar to the weighted composite statistic for schizophrenia in this DSM-5 Field Trial).[5][6]Research
Quotes
The DSM-5 on Boundaries Between Disorders
“Although some mental disorders may have well-defined boundaries around symptom clusters, scientific evidence now places many, if not most, disorders on a spectrum with closely related disorders that have shared symptoms, shared genetic and environmental risk factors, and possibly shared neural substrates (perhaps most strongly established for a subset of anxiety disorders by neuroimaging and animal models). In short, we have come to recognize that the boundaries between disorders are more porous than originally perceived.”– (DSM-5, Introduction, page 5)
The DSM-5 on Checklist Diagnoses
“The case formulation for any given patient must involve a careful clinical history and concise summary of the social, psychological, and biological factors that may have contributed to developing a given mental disorder. Hence, it is not sufficient to simply check off the symptoms in the diagnostic criteria to make a mental disorder diagnosis.”– (DSM-5, Use of the Manual, page 19)
– Freedman, Robert, et al. “The initial field trials of DSM-5: new blooms and old thorns.” (2013): 1-5.[7]
Beyond the DSM
ICD-10 and ICD-11
The International Statistical Classification of Diseases and Related Health Problems, also known as the ICD-10 is published by the World Health Organization, and commonly used outside of North America. The diagnostic criteria for the ICD-10 varies from the DSM-5 for a variety of mental disorders. The eleventh edition (ICD-11) is due to officially come into effect in January 2022.
Psychodynamic Diagnostic Manual (PDM)
The Psychodynamic Diagnostic Manual (PDM) is a diagnostic handbook that approaches mental disorders through a psychodynamic and humanistic lens. The 2nd version (PDM-2) was published in 2017.
Research Domain Criteria (RDoC)
The Research Domain Criteria (RDoC)[9] is a research framework proposed by the National Institute for Mental Health (NIMH) for new ways of studying and understanding mental disorders. It integrates many levels of information (from genomics to self-report) to better understand basic dimensions of functioning underlying the full range of human behaviour from normal to abnormal.
– Thomas Insel, National Institute of Mental Health Director, 2013
Hierarchical Taxonomy of Psychopathology (HiTOP)
Hierarchical Taxonomy of Psychopathology (HiTOP) is an alternative diagnostic system in development that deconstructs traditional diagnostic categories and recasts them in terms of a profile of dimensions. It remains underdevelopment at this time.