- Last edited on February 1, 2024
Attachment Theory
Primer
Attachment Theory is a psychological model that states strong emotional and physical attachment to at least one primary caregiver is critical in development during childhood. The theory posits that children are motivated to seek protective contact with caregivers, and if a parent responds sensitively to a child's distress, then the child feels secure enough to explore their environment.
What is Attachment?
Attachment defined as the particular emotional tie between an infant/child and a specific caregiver – particularly when the child is frightened, upset, tired or ill. In these instances, the child seeks security or comfort from the relationship with that specific caregiver.Epidemiology
- It is estimated that 62% of North American children have secure attachment.
Prognosis
- Healthy infant-parent attachment leads to optimal childhood development and also protects against adverse health outcomes
Theories of Attachment
The origins of attachment theory start with some key players. Psychiatrist John Bowlby proposed that attachment can be understood within an evolutionary context of how a caregiver provides safety and security for an infant. Attachment is seen as adaptive as it enhances an infant's chance of survival. Around the same time, psychologist Henry Harlow's early social isolation experiments on rhesus monkeys also showed experimental evidence for attachment.[1] Finally, Mary Ainsworth elaborated on Bowlby's initial work and took an experimental approach to observing a child's attachment to a caregiver.
Attachment Theorists
| Claim to Fame | Consequences of Theory | |
|---|---|---|
| Harry Harlow | Studied maternal deprivation, social isolation, and its effects in rhesus monkeys | Reinforced the importance of mother-and-child bonding. Also discovered that physiological needs (warmth, safety, food) alone are not enough, but also emotional needs are required (acceptance, love, affection). |
| John Bowlby | Coined “attachment behaviour” and founder of attachment theory | A child has an innate need to attach to one main attachment figure (i.e., monotropy, usually the mother). Believed mother-child attachment was an essential medium of human interaction. Attachment had important consequences for later development, personality, and risk of mental illness. Also coined the idea of an “internal working model,” where a child behaves according his representational system of self and other. This model originates from his relationship with his parent. |
| Mary Ainsworth | The “Strange Situation” experiment | Discovered that the interaction between mother and baby during attachment period significantly influences baby’s current and future behaviour. Maternal sensitivity and responsiveness are the main determinants of secure attachment. |
Ingredients for Attachment
- Infants must have a significant amount of interaction on a regular basis with a caregiver
- Infants must reach the 7 to 9 months mark (cognitive age) for the first signs of attachment behaviour to start occurring
Adverse Childhood Events (ACEs)
Adverse Childhood Experiences (ACEs) are traumatic events that occur during childhood (from age 0 to 17 years), and range from abuse and witnessing violence to growing up in a household with substance and mental health problems. Secure attachment is unlikely to happen in homes where there are multiple ACEs. For example, in a home where a primary caregiver is unavailable (e.g. - incarcerated, intoxicated, mentally ill), attachment between that caregiver and their child simply cannot occur, and insecure attachment is likely to occur.
Infant/Childhood Attachment Styles
The Strange Situation
The Strange Situation is an experimental procedure devised by Mary Ainsworth in the 1970s to observe attachment between a caregiver and a child. She found that infants typically followed one of four attachment styles.
Infant Behaviours in the Strange Situation
| Attachment Style as Child | Expected Behaviour From Caregiver | Description | Corresponding Attachment Style as Adult |
|---|---|---|---|
| Secure | Expects responsiveness | Explores rooms and toys with interest in pre-separation episodes. Shows signs of missing parent on separation, often crying by second separation. Obvious preference for parents over strangers. Greets parent actively, usually initiating physical contact. Usually some contact-maintaining by second reunion, but then settles and returns to play. | Secure/Autonomous |
| Insecure (Avoidant) | Expects rebuff (“I don’t want to show you I need you”) | Fails to cry on separation from parent, often continues to play even when left entirely alone. Actively avoids and ignores parent on reunion, i.e., moving away, turning away, or leaning out of arms when picked up. Little or no proximity or contact seeking, no distress, and no display of anger. Response to parent appears unemotional. Focuses on toys or environment throughout procedure. | Dismissive |
| Insecure (Ambivalent/Resistant) | Expects inconsistency (“I need you!”) | May be wary or distressed even prior to separation, with little exploration. Preoccupied with parent throughout procedure, may seem angry or passive during reunion. Following reunion, fails to settle and take comfort in parent, usually continuing to focus on parent and cry. Fails to return to exploration. | Preoccupied |
| Disorganized | Expects to be frightened/abused (“I love you, I hate you”) | The infant displays disorganized and/or disoriented behaviours in the parents presence. For example, the infant may freeze with a trance-like expression, may react unusually at parents entrance, may cling while crying hard, and/or leaning away with gaze averted. Infant may otherwise fit to secure, avoidant, or resistant categories. Typically infants will have a frightening or frightened parent and experience an environment that is felt as unpredictable and unsafe. | Unresolved/Disorganized (“dissociative symptoms”) |
These attachment styles can also be summarized in terms of the infant's view of self and view of others (see Table below), and reflects on what their attachment style will be when they become adults.
Infant Behaviour in the Strange Situation
| Positive view of self | Negative view of self | |
|---|---|---|
| Positive view of others | Secure (Higher self-esteem, higher sociability) | Anxious-ambivalent/resistant, insecure (Lower self-esteem, higher sociability) |
| Negative view of others | Anxious-avoidant, insecure (Higher self-esteem, lower sociability) | Disorganized/Disoriented (Lower self-esteem, lower sociability) |
Attachment and Attunement
Using attachment theory can inform how to approach children with attachment difficulties. For example, if a child's attachment style is “anxious” one can respond by being more supportive. Conversely, if a child has a “avoidant” style, one respond by promoting independence. This balanced response to the child's needs is called attunement, or simply put, you are responding to the child’s needs.Adult Attachment Styles
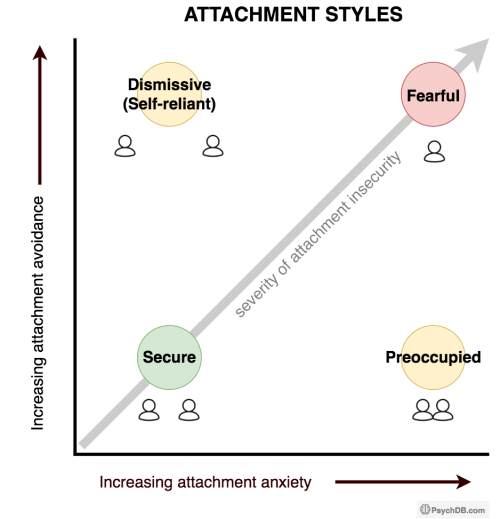
The attachment styles described above carry forward into adulthood. Adults can have one of four attachment styles:
Adult Attachment Styles
| Description | Summary | |
|---|---|---|
| Secure | Maintains appropriate closeness. Seeks out help when needed. | “I'm OK, you're OK” |
| Dismissive (Self-reliant) | Feels uncomfortable with closeness and deals with stress independently. Will avoid revealing of fear/neediness, and symptoms may be under-reported or suppressed. | “I'm OK, you're not OK” |
| Preoccupied | Feels uncomfortable being apart. Fears/symptoms may be more exaggerated, and tends to have a greater worry about health. | “I'm not OK, you're OK” |
| Fearful | Partners and caregivers experience contradictory signals, which can often be confusing and frustrating. | “I'm not OK, you're not OK” |
Attachment and Psychiatric Disorders
Insecure adult attachment is a strong transdiagnostic contributor to psychopathology in bipolar disorder, depression, and schizophrenia spectrum disorder.[2]
Attachment in Healthcare Settings
Video - Childhood Trauma, Adult Illness and the Need for a Health Care Revolution
When children become adults, they develop an internal working model that reflects these underlying attachment styles. Understanding a patient's attachment style when treating them as adults can help healthcare providers understand a patient's approach to healthcare and associated interventions/treatments. When one is ill or has a disease, attachment styles can be activated and play out in the healthcare provider-patient relationship. For example, individuals with anxious/dismissive attachment tend to have poorer health outcomes and treatment adherence, compared to those with secure attachment.[3] Being aware of patient's attachment styles as they present in a hospital or inpatient context can be helpful in managing challenging encounters (see Table below).
Adult Attachment Styles in Hospital Settings
| Presentation | Approach | |
|---|---|---|
| Secure | - | Care as usual |
| Dismissive | • Avoidant: “All conclusions, no facts.” Very little emotional content (e.g. -“Tell me about your dad “He’s a good dad.”) • Very quick and fast interviews, with very little affect. • Wants you to see them as not needing any help. | • Allow the patient to maintain their identity as an independent person as much as possible in the hospital setting • Involve patient as an equal partner in planning to ensure patient feels their right of self-determination (“I see you’re a self-reliant guy, you like to be independent.”) • Avoid rushing the patient into making decisions to allow them to have this autonomy • Empathize with how little independence the patient has when in a hospital or are unwell • Since patient may be reluctant to express symptoms, proactively check on symptoms and progress on a fixed schedule • Reframe medical care and procedures as pathway to regaining independence |
| Preoccupied | • Anxious incoherence: “All facts, but no conclusions.” “Never finishes a sentence.” There may be lots of affect. • Primary drive and purpose of communication is to not be alone, will say whatever to maintain this (hypersignaling). • These presentations tend to wear on providers, and paradoxically causes more distance. | • This patient’s understanding of the healthcare system. Provide care on a schedule, to make it reliable and predictable. • Pre-empt distress by breaking the link that distress is associated with care • Telling the patient who their primary caregiver is at the start of each shift • Provide regular check-ins (e.g. - q30 minutes for RN staff), but defer all but urgent care if patient requests help in between check-ins • This regular check-in allows patients to learn that hospital staff can respond reliably, and become less demanding from this position of reassurance • Teach patient non-pharmacological coping strategies (e.g. - mindfulness and relaxation techniques) |
| Fearful/Disorganized | Unpredictable | • Provide usually excellent level of care (capacity for patient to disorganize the team is high) • Ask patient “what can we do to make you feel safer in this environment?” • Reduce situations that might increase a patient's sense of threat • Help the treating team understand the patient's behaviours, and develop empathy for the patient's behaviours • Reduce the frequency of sudden, unpredictable, or fearful events • Limit the number of staff involved in the patient's care (whenever possible) • Collaborate with patient's trusted contacts (e.g. - family doctor) if possible |
Adult Attachment Interview (AAI)
The Adult Attachment Interview (AAI) is an important tool in attachment research and clinical use, and uses 20 open-ended questions about an individual's recollection of their own childhood. What is powerful about the AAI is that it is highly effective at predicting how a child of the adult interviewee would be attached to his/her parent (with more than 80 percent predictability).[4] The AAI provides an empirically validated method to follow the transmission of attachment patterns from generation to generation.
Attachment Scales
| Name | Rater | Description | Download |
|---|---|---|---|
| Adult Attachment Interview (AAI) | Clinician/Patient | 20 open-ended questions about an individual's recollection of their own childhood | Download |