- Last edited on January 28, 2022
Malingering
Primer
Malingering is the intentional production false or grossly exaggerated physical or psychological complaints with the goal of receiving a reward. Malingering is not a mental disorder or diagnosis.
Incidence
- The true rates of malingering is difficult to determine, as the nature of malingering involves deception.
- There is estimated to be a prevalence of 1% in psychiatric patients, 5% in military personnel, and between 10 to 20% in medicolegal cases.[1]
- The incidence of malingering in forensic assessment settings is as high as 50%.[2]
Not a Diagnosis
- Malingering is not a diagnosis, even though it is encountered in the clinical setting.
- To establish malingering is difficult. Symptoms from malingering are intentional, and the motivation behind it is also intentional.
- The individual consciously fakes, profoundly exaggerates, or claims to have a disorder or symptoms in order to attain a specific secondary (external) gain.
- This gain could be avoiding work, getting worker's compensation, or obtaining something of material value. Complaints from malingerers will end after they have achieved their gain (in comparison to factitious disorder, which is not always the case).
Assessment
Detecting Malingering
- Even health professionals and professional “lie detectors” (e.g. - police officers, judges, border officers) are very poor at detecting malingering in most cases.[3]
- More structured and detailed psychometric testing may aid in improving detection, using detailed tests such as the:
- Structured Interview of Reported Symptoms (SIRS)
- Minnesota Multiphasic Personality Inventory, Revised (MMPI-2)
- Miller Forensic Assessment of Symptoms Test (M-FAST)
Cognitive
Individuals with malingering may feign cognitive impairment; several tests to detect for cognitive malingering include:
- Coin-in-hand test[4]
- Tests of Memory Malingering (TOMM)[5]
- Rey Fifteen-Item Test (FIT)
- With this test, the clinicians detects whether there is a “floor effect”, which assumes the individual attempting to malinger will fail at a task which even a grossly impaired individuals are likely to perform adequately.
- Word Memory Test (WMT)
Conversion Disorder vs. Malingering*
| Malingering | Conversion Disorder |
|---|---|
| • Malingering: Aware of purpose of symptoms • Usually uncooperative, suspicious, aloof • Avoids examinations and investigations (unless there is a financial benefit) • Refuses employment with partial disability • Describes accident in full “perfect” detail | • Not aware of purpose of their symptoms • Cooperative, appealing, and more dependent • Welcomes examinations and investigations • Accepts employment with partial disability • Describes accident with gaps and inaccuracies |
Delusions and Hallucinations
See also:
- Individuals may also feign psychotic symptoms such as hallucinations or delusions.
- If a patient alleges unusual hallucinations, ask about them in detail. There are several key things to note:[6]
- Hallucinations are almost always associated with delusions.
- Genuine hallucinations are typically intermittent rather than continuous.
- In schizophrenia, the major themes are persecutory or instructive (command).[7]
- Auditory hallucinations are usually clear, not vague (7%) or inaudible
- Both male and female voices are commonly heard (75%)
- Voices are usually perceived as originating outside the head (88%)
- Real hallucinations tend to diminish when patients are involved in activities (patients typically cope by engaging in activities, changing posture, seeking interpersonal contact, taking medication)
- Visual hallucinations are experienced by an estimated 24% to 30% of psychotic individuals but are reported much more often by malingerers (46%) than by persons with genuine psychosis (4%)
- True visual hallucinations are usually of normal size and in colour
- Timeline of symptoms:
- Malingerers may claim that a delusion began or disappeared suddenly.
- In reality, systematized delusions usually take weeks to develop and much longer to disappear.
- Other features:
- Malingerers are more likely to give vague or “hedge” their answers to straightforward questions.
- Malingerers are more likely to eagerly “thrust forward” their illness, whereas patients with schizophrenia are often reluctant to discuss their symptoms.
Uncommon Psychotic Presentations
Adapted from: Resnick, P. J., Knoll, J. (2005). Faking it: How to detect malingered psychosis. Current Psychiatry, 4(11), 12.| Hallucinations | Delusions |
|---|---|
| • Continuous • Voices are vague, inaudible • Hallucinations are not associated with delusions • Voices use stilted language • Patient uses no strategies to diminish or cope with hallucinations • Patient states that they obey all commands • Visual hallucinations in black and white • Visual hallucinations alone in schizophrenia • Visual hallucinations are exaggerated in size (very small or very large) | • Sudden/abrupt onset or termination • Patient's behaviour is inconsistent with delusions • Bizarre content without disorganization • Patient is overly eager to discuss delusions |
Other Diagnoses
-
- Malingering should not be considered until all other diagnoses have been considered!
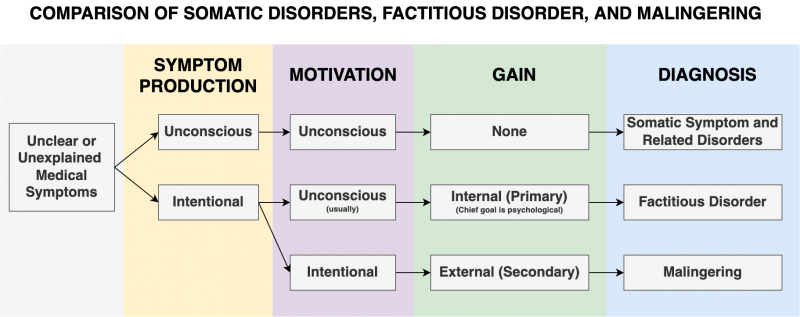
Comparison of Somatic Disorders
References
1)
Benjamin JS, Virginia AS (editors): Kaplan & Sadock's Synopsis of Psychiatry, Ed 10. Philadelphia, Lippincott Wiliams & Wilkins, 2007.
2)
Ardolf, B. R., Denney, R. L., & Houston, C. M. (2007). Base rates of negative response bias and malingered neurocognitive dysfunction among criminal defendants referred for neuropsychological evaluation. The Clinical Neuropsychologist, 21(6), 899-916.
3)
Walczyk, J. J., Sewell, N., & DiBenedetto, M. B. (2018). A review of approaches to detecting malingering in forensic contexts and promising cognitive load-inducing lie detection techniques. Frontiers in psychiatry, 9, 700.
4)
Kapur, N. (1994). The coin-in-the-hand test: a new" bed-side" test for the detection of malingering in patients with suspected memory disorder. Journal of neurology, neurosurgery, and psychiatry, 57(3), 385.
5)
Walczyk, J. J., Sewell, N., & DiBenedetto, M. B. (2018). A review of approaches to detecting malingering in forensic contexts and promising cognitive load-inducing lie detection techniques. Frontiers in psychiatry, 9, 700.