- Last edited on May 7, 2021
Illness Anxiety Disorder
Primer
Illness anxiety disorder is a mental disorder characterized by a preoccupation with having or acquiring a serious, undiagnosed medical illness. Somatic symptoms are either not present or mild in intensity. Illness anxiety can be thought of as a generalized anxiety disorder that focuses exclusively on health concerns.
Epidemiology
- Individuals with illness anxiety disorder are encountered far more frequently in primary care and specialist medical settings than in mental health or psychiatric settings.
- Prevalence (based on old estimates from DSM-III and DSM-IV diagnosis hypochondriasis) is 1.3% to 10%.
- In ambulatory medical populations, the prevalence is between 3% and 8%.
- The prevalence is equal between and males and females.
Prognosis
- The course of illness anxiety disorder is unclear. It is considered to be a chronic and relapsing condition with onset in early and middle adulthood.
- In older individuals, health-related anxiety may focus on memory loss (i.e. - subjective memory impairment).
- Between one-third to one-half of individuals with illness anxiety disorder have a transient form that is less severe, and associated with less psychiatric comorbidity.
Comorbidity
- Exact comorbidities are not well defined since illness anxiety is a new diagnosis. Based on the hypochondriasis diagnosis, there is comorbidity with anxiety disorders including generalized anxiety disorder, panic disorder, and obsessive compulsive disorder.
- Additionally, the likelihood of somatic symptom disorder and personality disorders are also thought to be increased. 66% of individuals with illness anxiety disorder are likely to have at least one other comorbid psychiatric disorder.
- Cluster C personality disorders are also more common.[1]
Risk Factors
- Illness anxiety can be precipitated by a major life stress or a serious but ultimately benign threat to the individual's health. Other risk factors include childhood abuse, or serious childhood illnesses.
Cultural
The diagnosis should be made with caution in individuals whose ideas about disease are congruent with widely held, culturally sanctioned beliefs. The phenomenology of illness anxiety disorder across culture is not well understood.
History
DSM-IV to DSM-5 Changes
- Somatic symptom disorder is a new diagnosis in the DSM-5.
- Individuals previously diagnosed with somatisation disorder, hypochondriasis, pain disorder, and/or undifferentiated somatoform disorder are typically subsumed under this new diagnosis.
- The lumping of these diagnoses has not been without controversy.[2]
- About 25% of individuals with the old DSM-IV diagnosis of hypochondriasis are now diagnosed with illness anxiety disorder. This applies when they do not have prominent somatic symptoms.
- The other 75% of hypochondriasis are subsumed under the diagnosis of somatic symptom disorder.
DSM-5 Diagnostic Criteria
Criterion A
Preoccupation with having or acquiring a serious illness.
Criterion B
Somatic symptoms are not present or, if present, are only mild in intensity. If another medical condition is present or there is a high risk for developing a medical condition (e.g. - strong family history is present), the preoccupation is clearly excessive or disproportionate.
Criterion C
There is a high level of anxiety about health, and the individual is easily alarmed about personal health status.
Criterion D
The individual performs excessive health-related behaviours (e.g. - repeatedly checks body for signs of illness) or exhibits maladaptive avoidance (e.g. - avoids doctor appointments and hospitals).
Criterion E
Illness preoccupation has been present for at least 6 months, but the specific illness that is feared may change over that period of time.
Criterion F
The illness-related preoccupation is not better explained by another mental disorder, such as somatic symptom disorder, panic disorder, generalized anxiety disorder, body dysmorphic disorder, obsessive-compulsive disorder, or delusional disorder, somatic type.
Specifiers
Specifiers
Specify whether:
- Care-seeking type: Medical care, including physician visits or undergoing tests and procedures, is frequently used.
- Care-avoidant type: Medical care is rarely used.
Signs and Symptoms
- In illness anxiety disorder, a thorough evaluation fails to identify a serious medical condition that accounts for the individual's concerns.
- While the concern may be originate from a non-pathological physical sign or sensation, the individual's distress comes not primarily from the physical issue itself but rather from the anxiety about the meaning, significance, or cause of the complaint (i.e. - the suspected medical diagnosis).
- The concern about undiagnosed disease does not respond to appropriate medical reassurance, negative diagnostic tests, or benign course.
- Individuals may research their suspected disease excessively (e.g. - on the Internet) and repeatedly seek reassurance from family, friends, or physicians.
- This worrying can in some cases become frustrating for others and cause interpersonal strain.
Pathophysiology
Differential Diagnosis
- Other medical conditions
- The first differential diagnostic consideration is an underlying medical condition, including neurological or endocrine conditions, occult malignancies, and other diseases that affect multiple body systems. If a medical condition is present, the health-related anxiety and disease concerns are clearly disproportionate to its seriousness. Transient preoccupations related to a medical condition do not constitute illness anxiety disorder. The presence of a medical condition does not rule out the possibility of coexisting illness anxiety disorder.
- Adjustment disorders or non-pathological health anxiety
- Health-related anxiety is a normal response to serious illness and is not a mental disorder. Such non-pathological health anxiety is clearly related to the medical condition and is typically time-limited. If the health anxiety is severe enough, an adjustment disorder may be diagnosed. However, only when the health anxiety is of sufficient duration, severity, and distress can illness anxiety disorder be diagnosed. Thus, the diagnosis requires the continuous persistence of disproportionate health-related anxiety for at least
6months.
-
- Somatic symptom disorder is diagnosed when significant somatic symptoms are present. In contrast, individuals with illness anxiety disorder can only have mild or minimal somatic symptoms and are primarily concerned with the idea they are ill.
-
- In generalized anxiety disorder, individuals worry about multiple events, situations, or activities, only one of which may involve health. In panic disorder, the individual may be concerned that the panic attacks reflect the presence of a medical illness; however, although these individuals may have health anxiety, their anxiety is typically very acute and episodic. In illness anxiety disorder, the health anxiety and fears are more persistent and enduring. Individuals with illness anxiety disorder may experience panic attacks that are triggered by their illness concerns.
-
- Individuals with illness anxiety disorder may have intrusive thoughts about having a disease and also may have associated compulsive behaviours (e.g. - seeking reassurance). However, in illness anxiety disorder, the preoccupations are usually focused on having a disease, whereas in obsessive-compulsive disorder (OCD), the thoughts are intrusive and are usually focused on fears of getting a disease in the future. Most individuals with OCD have obsessions or compulsions involving other concerns in addition to fears about contracting disease. In body dysmorphic disorder, concerns are limited to the individual's physical appearance, which is viewed as defective or flawed.
-
- Some individuals with depression may ruminate about their health and worry excessively about illness. A separate diagnosis of illness anxiety disorder is not made if these concerns occur only during major depressive episodes. However, if excessive illness worry persists after remission of the episode, a diagnosis of illness anxiety disorder should be considered.
-
- Individuals with illness anxiety disorder are not delusional and can acknowledge the possibility that the feared disease is not present. Their ideas do not have the same fixed rigidity and intensity seen in the somatic delusions occurring in psychotic disorders (e.g. - schizophrenia, delusional disorder, somatic type, or major depressive disorder with psychotic features). True somatic delusions are generally more bizarre (e.g. - that an organ is rotting or dead) than the concerns seen in illness anxiety disorder. The concerns seen in illness anxiety disorder, though not founded in reality, are plausible.
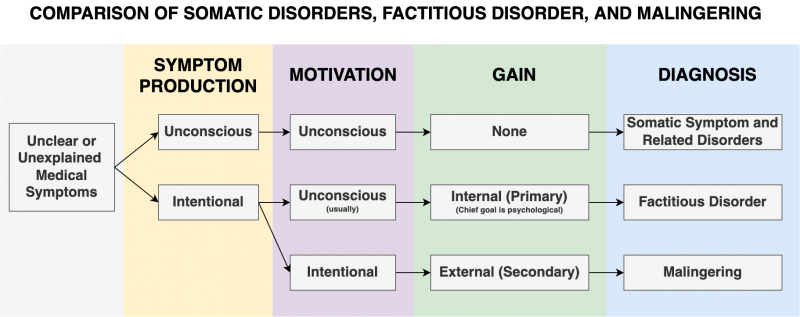
Comparison of Somatic Disorders
Investigations
Physical Exam
Treatment
Education and Follow Up
- Regularly scheduled follow up appointments, non-contingent on the presence of symptoms may be helpful.
- Avoid unwarranted investigations, treatment, and medications (“de-medicalize” interactions when appropriate)
- Avoid invalidating the patient's experiences
Psychotherapy
- Exposure therapy
Pharmacotherapy
- Based on prior evidence from hypochondriasis, SSRIs such as fluoxetine may be an effective treatment.[3]